How to Read Your EOB Line by Line (And Avoid Overpaying)
Master your Explanation of Benefits with our complete step-by-step guide. Learn what every line means, calculate your patient responsibility, and spot billing errors before paying.
Our medical bill checker analyzes your medical bills for errors, duplicate charges, and overcharges in seconds. Use our EOB comparison tool to compare your provider bill to your insurance statement instantly.
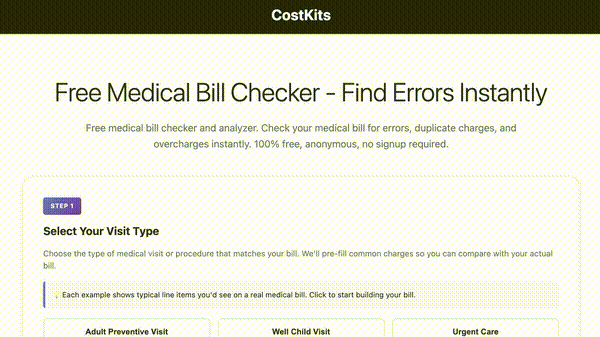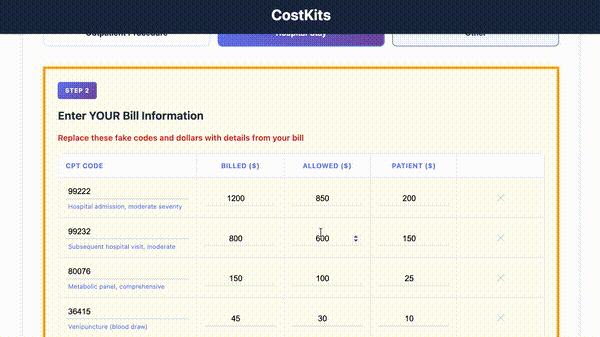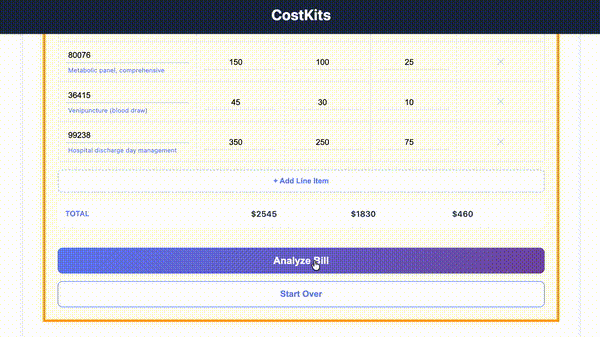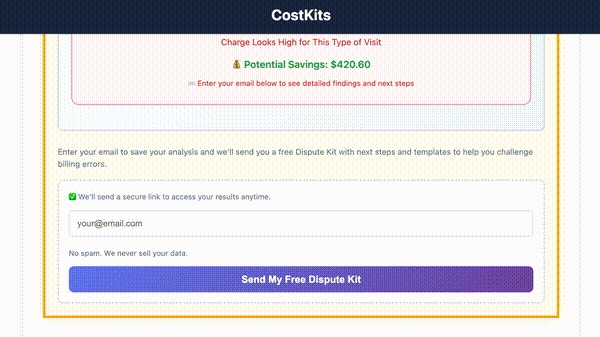
Enter line items from your medical bill and get instant analysis. Save your results with email.
We recently published a detailed guide explaining what happens if you don't pay a medical bill , including timelines, collections, and your consumer rights.
Check bills & save your analysis
Catch billing errors before you pay
Common signs of medical bill errors include duplicate charges, incorrect procedure codes, charges for services not received, and amounts that don't match your Explanation of Benefits (EOB). Our free checker identifies these instantly. Learn more about reading your medical bill →
Yes! CostKits offers a completely free medical bill checker that analyzes your bills for errors, duplicate charges, and overcharges. No signup, no credit card, and 100% anonymous. Enter your bill details or email your bill to get instant analysis.
The most common errors include duplicate charges (same service billed twice), upcoding (billing for more expensive procedures), unbundling (charging separately for services that should be combined), and charges for services not received. See real examples of billing errors →
Your EOB comes from your insurance and shows how they processed your claim. Your medical bill is from the provider requesting payment. Comparing them helps catch errors. Read our complete EOB vs Medical Bill guide →
Medical bills follow a specific timeline. Most providers give you 30-180 days before collections begins. You have rights under the FDCPA once collectors are involved. Learn the collections timeline and your rights →
Yes. We are HIPAA compliant and use bank-level encryption to protect your medical information. Your data is never shared with third parties without your explicit consent.
Your bill amount depends on three things: (1) the CPT code billed, (2) your insurance's negotiated rate (which is 30-70% less than the provider's list price), and (3) your deductible/coinsurance status. The same $500 service might cost you $50-$2,000 depending on these factors. That's why price transparency matters—and why CostKits analyzes what you *should* be paying versus what's actually billed.
Your "allowed amount" is the negotiated rate your insurance company has agreed to pay the provider—typically 30-70% less than the provider's chargemaster (list price). Your bill should never exceed the allowed amount if the provider is in-network. If it does, that's a billing error. CostKits catches these automatically and flags them for dispute.
Balance billing happens when an in-network provider illegally bills you for the difference between their chargemaster and your insurance's allowed amount. Look for items where "Patient Responsibility" exceeds your deductible plus coinsurance. This is a violation of the No Surprises Act. CostKits flags these as potential overcharges so you can dispute them with your insurance and get a refund.
You have options: (1) Contact the provider's billing department to negotiate or set up a payment plan—many offer 0% interest. (2) File an appeal if you believe the bill contains errors (use CostKits to identify them). (3) Know your rights: as of January 2025, medical debt can't appear on your credit report, so don't ignore the bill out of fear. Get errors fixed *before* debt spirals.
Yes—if the error is confirmed. Refunds typically take 30-90 days after you dispute in writing. Common refund reasons: duplicate charges, unbundling errors (splitting one service into multiple codes), charges for services not rendered, or amounts exceeding the allowed rate. CostKits identifies these errors instantly so you can file a dispute. Document everything: your EOB, bill, and error analysis. Providers refund 75%+ of disputes when challenged properly.